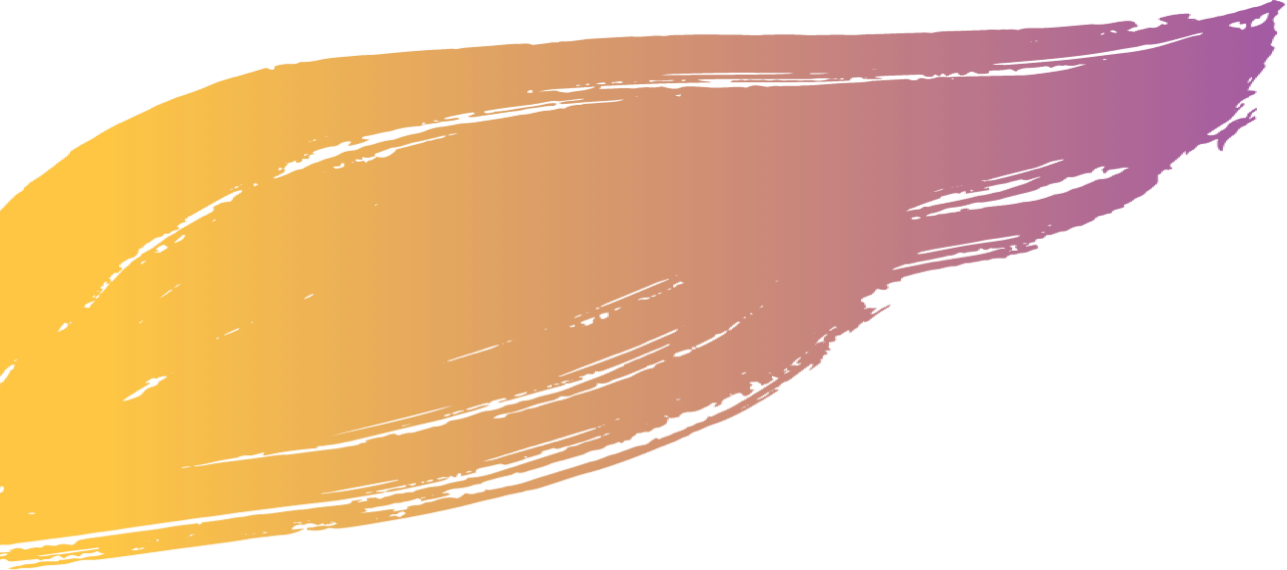
- This is not an all-inclusive listing. Adapted from Younossi ZM, Bernstein D, Shiffman ML, et al. Am J Gastroenterol. 2019;114(1):48-63.
Primary Biliary Cholangitis (PBC) Predictive Biomarkers
Despite no consensus on response criteria, ALP and bilirubin have been considered the most important biomarkers in managing risk1-4
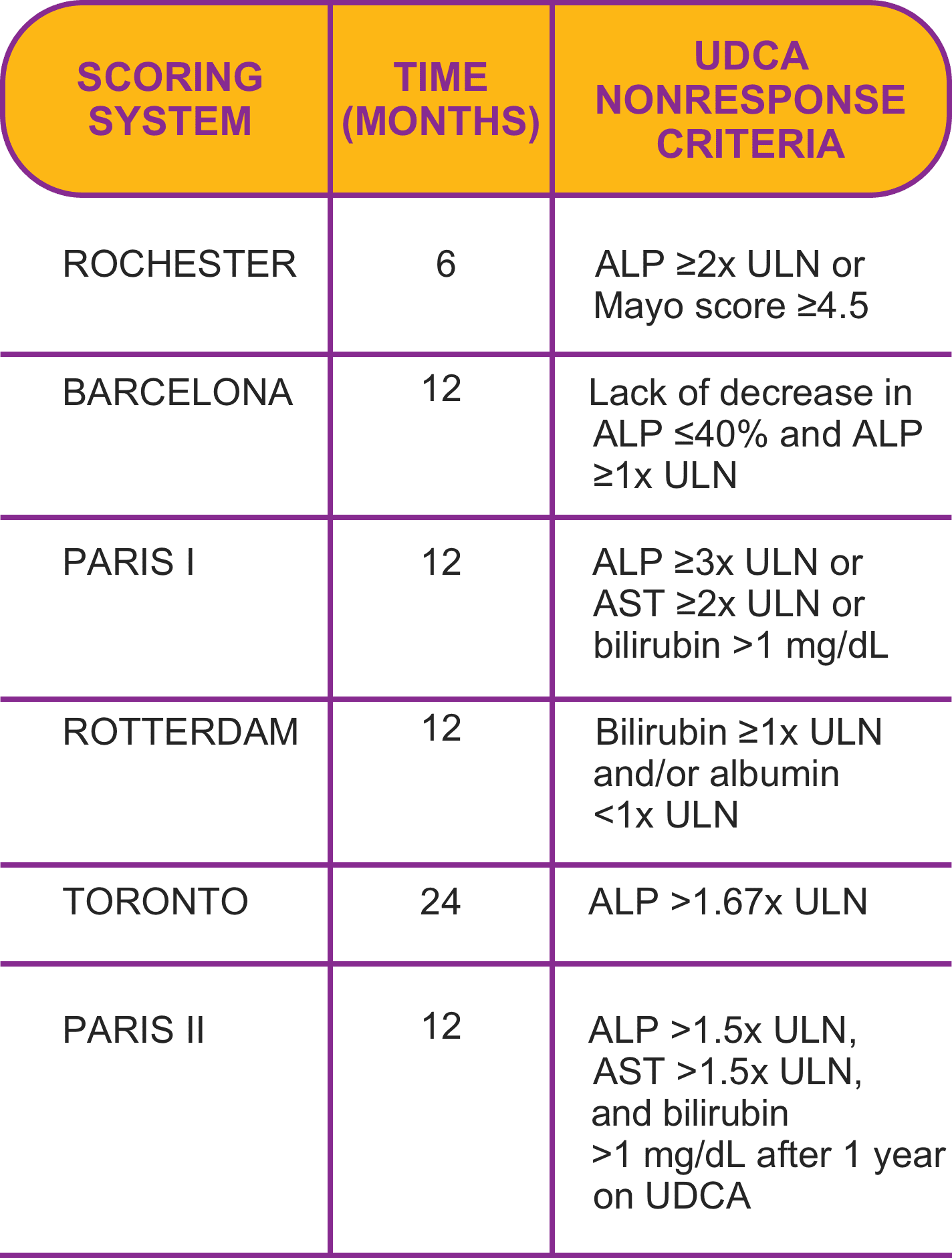

Risk of progression is dependent on reduction of predictive biomarkers3,5
- Prior to first-line treatment, patients may have ALP 4x-5x ULN and bilirubin above normal6,a
- Levels of ALP and bilirubin measured at baseline and each year for 5 years are strongly associated with clinical outcomes (liver transplant or death)5,b
Elevations in ALP and bilirubin have been found to have a considerable impact on liver transplant or death7,c
Occurrence of liver transplant or death
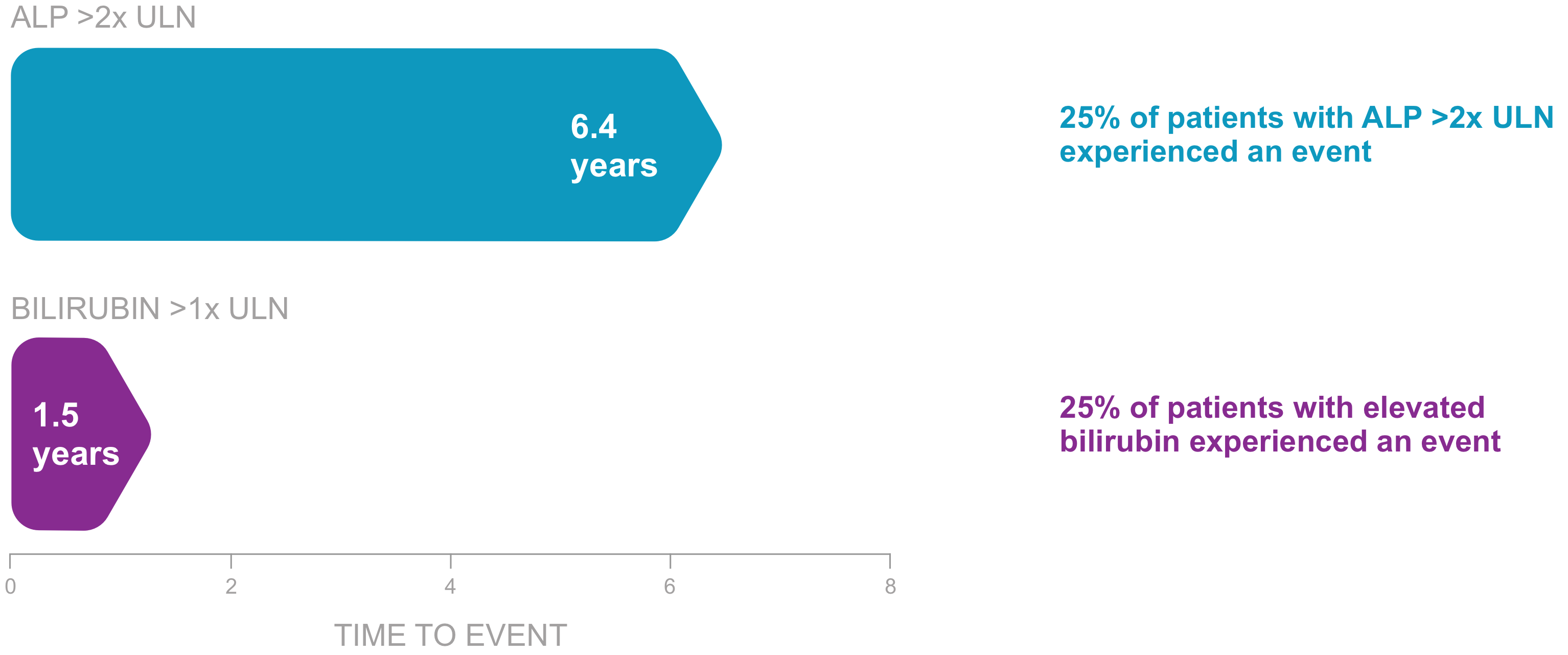
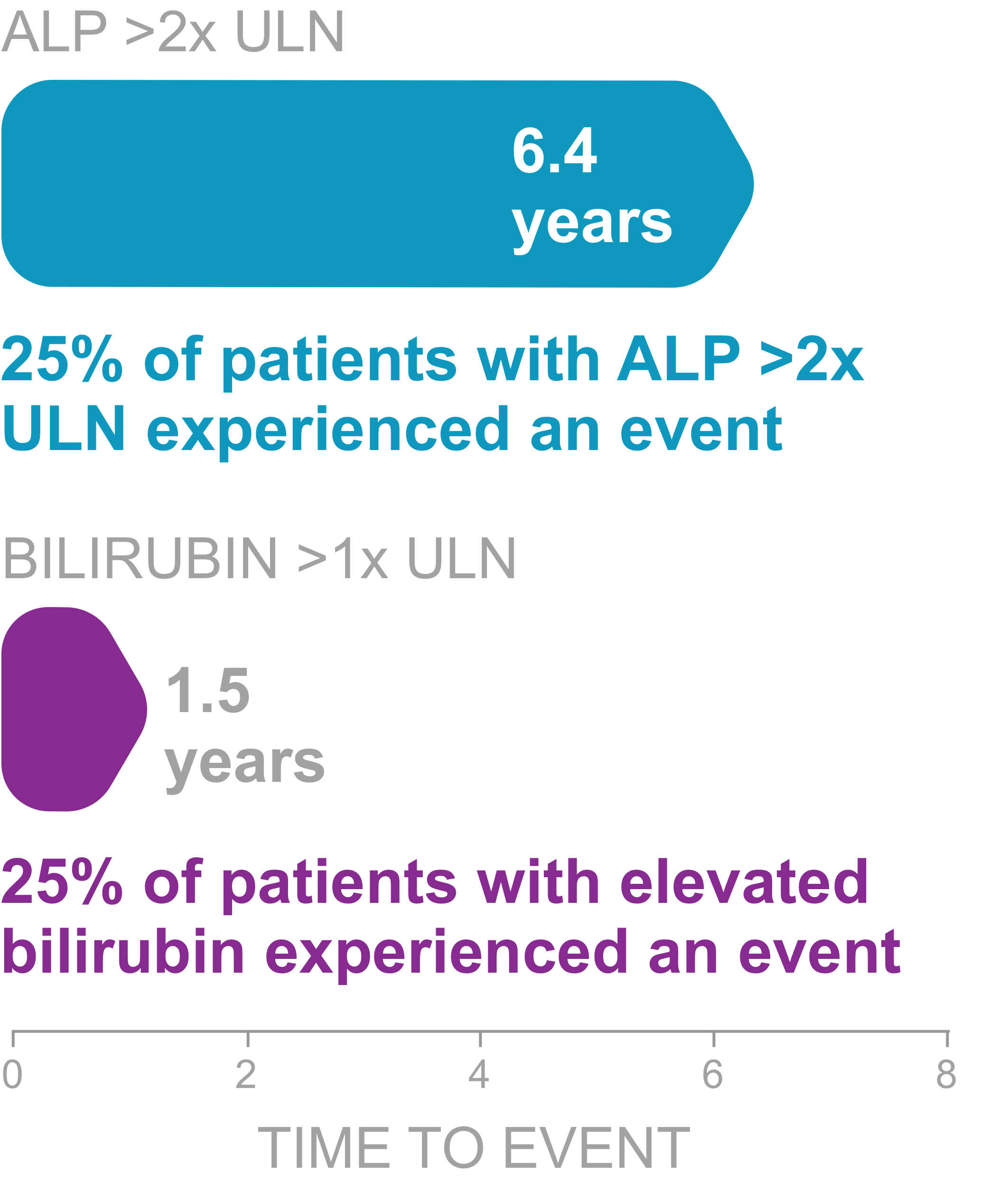
Elevations in ALP increase risk of poor outcomes7
ALP >2x ULN is associated with a 2.2x greater risk for liver transplant or death at 1 year compared to those who remained ≤2x ULN (P<.0001)
Higher bilirubin levels are associated with increased mortality and reduced transplant-free survival7
Bilirubin >1x ULN is associated with a 5.5x greater risk for liver transplant or death at 1 year (P<.0001)
- a Data from a combined analysis of 3 randomized, controlled trials comparing UDCA (n=273) vs placebo (n=275) for up to 4 years.6
- b Data from an international, multicentered meta-analysis of UDCA-treated and untreated patients diagnosed with PBC (N=4,845).5
- c Patient data were obtained from the international Global PBC study database; specifically, this analysis included UDCA-treated patients who had ALP ≤2x ULN or bilirubin ≤1x ULN at 1 year follow-up (N=2,527) who were evaluated to identify patients within this group at risk for adverse outcome during follow-up (median follow-up of 7.11 years).7
- ALP, alkaline phosphatase; AST, aspartate aminotransferase; UDCA, ursodeoxycholic acid; ULN, upper limit of normal.
References:
1. Murillo Perez CF, Hirschfield GM, Corpechot C, et al; the GLOBAL PBC Study Group. Fibrosis stage is an independent predictor of outcome in primary biliary cholangitis despite biochemical treatment response. Aliment Pharmacol Ther. 2019;50(10):1127-1136. 2. Younossi ZM, Bernstein D, Shiffman ML, et al. Diagnosis and management of primary biliary cholangitis. Am J Gastroenterol. 2019;114(1):48-63. 3. Lindor KD, Bowlus CL, Boyer J, Levy C, Mayo M. Primary biliary cholangitis: 2018 practice guidance from the American Association for the Study of Liver Diseases. Hepatology. 2019;69(1):394-419. 4. European Association for the Study of the Liver. EASL clinical practice guidelines: management of cholestatic liver diseases. J Hepatol. 2009;51(2):237-267. 5. Lammers WJ, van Buuren HR, Hirschfield GM, et al; the Global PBC Study Group. Levels of alkaline phosphatase and bilirubin are surrogate end points of outcomes of patients with primary biliary cirrhosis: an international follow-up study. Gastroenterology. 2014;147(6):1338-1349. 6. Poupon RE, Lindor KD, Cauch-Dudek K, Dickson ER, Poupon R, Heathcote EJ. Combined analysis of randomized controlled trials of ursodeoxycholic acid in primary biliary cirrhosis. Gastroenterology. 1997;13(3):884-890. 7. Lammers WJ, Van Buuren HR, Ponsioen CY, et al. Elevation of alkaline phosphatase during follow-up is an early predictor of hyperbilirubinaemia and of clinical endpoints in primary biliary cholangitis – an international study. Poster presented at: 66th Annual Meeting of the AASLD; November 13-15, 2015; San Francisco, CA.